You might not believe your jaw is the reason for a headache. However, TMJ (temporomandibular joint) could be the culprit.
Your jaw connects to your skull via the TMJ. It allows you to talk, laugh, chew, and allow your jaw to move side-to-side and up/down.
This joint is more complex than most other joints and can lead to headaches due to its sliding and hinge motions. These are commonly called Temporomandibular Disorders (TMD).
Table of Contents
What is TMJ Headache?
TMJ stands for Temporomandibular Joint. TMJ headaches can be understood to refer to Temporomandibular joint headaches.
TMJ Headaches is a common TMJ disorder. TMJ disorders can sometimes cause headaches. Other times, they can occur as secondary causes.
TMJ disorders are known for causing a dull, aching headache. It’s most common on one side but it can also be on both. It is usually worse on the side with the TMJ.
Jaw movement can aggravate headaches and jaw relaxation can relieve it. The headache is often accompanied by tenderness in the jaw and other nearby muscles.
Migraines, on the other hand, are more sharp and throbbing. These symptoms can also cause vision and sensation problems. TMJ disorders may make migraines more frequent, but they don’t directly cause them. Headaches aren’t always specific to one condition.
Any headache can lead to serious conditions. It is easier to diagnose headaches if you have TMJ symptoms. If other TMJ symptoms do not exist or the headache is not typical for TMJ, it is a good idea to seek medical attention.
TMJ syndromes can cause headaches. This is because inflammation and swelling in the temporomandibular joints travel to other muscles and ligament tissues in your jaw area.
It spreads and causes muscle spasms. It can cause headaches in the neck, skull, and face areas. TMJ disorders can sometimes cause headaches due to asymmetry in the alignment of the jaws.
Tension headaches can also be caused by joint and muscle stress.
It is crucial to monitor the company that has headaches due to TMJ disorders. It’s reassuring to know if other symptoms of TMJ are present. If they are not, it is less important.
TMJ syndromes can cause headaches, which is why it is important to seek treatment.
TMJ Headache Location

Other headaches only affect the head. TMJ headaches can cause pain in the cheeks, ears, and jaw, as well as the top of your head. TMJ headaches can cause severe pain in the neck and shoulders.
TMJ headache relief
TMJ pain can sometimes be treated with nonsteroidal anti-inflammatory medication (NSAIDs). This is a short-term treatment that reduces jaw pain and headaches. These medications include Aspirin (Excedrin), ibuprofen, and naproxen. You can also relieve pain by icing your jaw.
What causes TMJ headache?
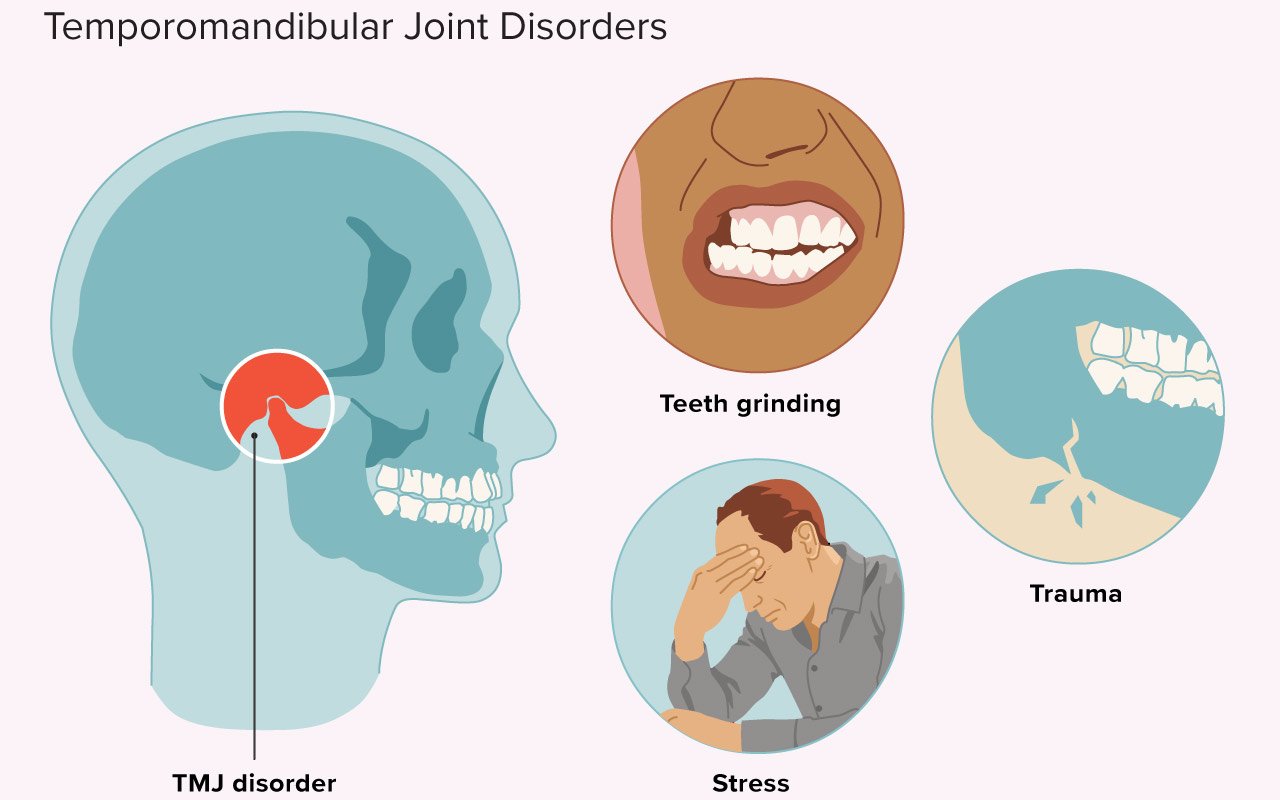
TMD can be caused by teeth grinding or constant tooth grinding. TMJ pain has been reported in 1 out 10 people. TMD has also been reported in nearly half the US population.
TMJ headaches are not well-studied because it is difficult to differentiate between them.
Your jaw and cheek muscles are connected by the TMJ muscles. Sometimes, these muscles can cause pain and even headaches. A headache can occur when the tension in your jaw muscles causes you to grind your teeth.
TMJ problems such as osteoarthritis, joint hypermobility, or osteoporosis can also cause headaches.
The connection between TMJ and headaches
TMJ connects directly to your head and secures your jaw to the head. TMJ is associated with muscles in various parts of your face, including the cheeks, jaws, and head.
TMJ disorder can trigger a painful headache if any of these muscles become tightened. TMJ disorder can be caused by misalignment, an uneven bite, hormonal imbalance, or mental stress.
If you pay attention, other headaches can be distinguished from TMJ headaches. In the next sections, we will discuss how to identify a TMJ headache as well as conventional TMJ headache treatment options.
TMJ headache symptoms
TMJ headaches can be caused by many things, but they are most often accompanied by other symptoms.
Here is a list of symptoms of TMJ headache. These symptoms usually do not occur if your headache is caused by another cause.
- Clicking and Popping Sound from Mouth
- Chewing can be difficult and painful.
- Pain in the Ears and Other Parts of The Face
- Ringing in the Ears and Hearing Loss
- Jaw Movements are difficult
- TMJ pain
- Abnormality in Bite
- Jaw Movements Cause Headaches
- Teeth clenching
- Muscles in the jaw or facial area should be tight
- A jaw or facial pain
- A clicking sound in the jaw
- Restricted movement of the jaw
- Changes in your bite, that is, how your top and bottom teeth fit together.
TMJ headaches can also recur in certain areas of the head or feel like tension headaches.
9 Best TMJ Exercises for Pain Relief
TMJ exercises are not known to relieve pain. They are believed to be helpful:
- strengthen jaw muscles
- Stretch the jaw
- Relax your jaw
- Increase jaw mobility
- reduce jaw clicking
- promote jaw healing
One study from 2010 that was published in the Journal of Dental Research found that TMJ exercises increase mouth opening range in people with TMJ disc dislocation.
These nine exercises by the American Academy of Family Physicians and the Royal Surrey County Hospital can help to relieve TMJ pain and improve the movement of your jaw joints.
Frequency recommendations are available for some exercises. Ask your dentist or doctor for assistance if frequency recommendations are not available.
1. Relaxed jaw exercise
Place your tongue on the roof of your mouth, just behind your upper front teeth. Relax your jaw muscles and allow your teeth to fall apart.
2. Goldfish exercises (partial opening)
Your tongue should be on the roof of your mouth. One finger should be in front of your TMJ. Place your pointer or middle finger on your chin. Your lower jaw should be dropped halfway. Close your eyes.
You should feel some resistance, but not pain. Another variation is to place one hand on each TMJ and then drop your lower jaw halfway. Close the mouth again. Repeat this six times.
3. Exercises with Goldfish (full opening).
Keep your tongue on the roof and place one finger on each side of your TMJ. The other finger should be on your chin. Your lower jaw should be completely dropped and then retracted.
You can also do this exercise by placing one finger on each TMJ. This will allow you to completely drop your lower jaw. To complete one set, repeat the exercise six times.
Each set should be completed six times per day.
4. Chin tucks
Keep your shoulders back and your chest up. Next, draw your chin back to create a “double-chin”. Hold the position for three seconds, then repeat 10 times.
5. Resist opening the mouth
Your thumb should be under your chin. For resistance, open your mouth slowly and press gently against your chin. For three to six seconds, hold the position and then slowly close your mouth.
6. Resisted closing the mouth
With one hand, press your chin gently with your thumb and index. As you gently press down on your chin, close your mouth. This will strengthen the muscles that allow you to chew.
7. Tongue up
Slowly open your mouth while your tongue touches the roof of your mouth.
8. Side-to-side jaw movement
Place a 1/4-inch object (e.g. stacked tongue depressors) between your front teeth and move your jaw slowly from one side to the other. You can increase the thickness between your teeth by stacking them on top of one another.
9. Forward jaw movement
Placing a 1/4-inch object between your front teeth is a good idea. Your bottom jaw should be moved forward so that your bottom teeth are in front of your top teeth.
You can increase the distance between your teeth as the exercise becomes easier.
TMJ Headache Treatment
Your dentist should be consulted if you suspect that you have a TMJ disorder. The dentist will be able to diagnose the problem. Below are some options for treating TMJ headaches.
Medical treatment
Depending on your medical condition, doctors may prescribe strong medication. A bite guard (mouthguard) may also be recommended by your doctor.
TMJ headaches are often associated with clenching and grinding teeth. Protect your teeth with a bite guard to prevent clenching and other harmful effects.
Talk to your doctor if non-invasive or conservative treatments aren’t effective. Your doctor may recommend something stronger to relieve the pain of a bite guard (stabilization splint). A stabilization splint can be prescribed by your dentist.
TMJ is treated with splints. They can protect your teeth from grinding, but they aren’t proven to alleviate pain.
These treatments, like the ones mentioned before, are temporary and reversible. These should not be considered permanent solutions.
TMJ disorder can be treated with medications and bite guards, but they are not permanent. If you don’t pay attention and take the proper precautions, your condition could become worse.
TMJ lifestyle & TMJ diet
TMJ headache relief can be achieved by lifestyle changes. Reduce stress. To calm your nerves, you can do breathing exercises, yoga, and meditation.
TMJ disorder patients should keep their jaws soft and slow. Avoid excessive jaw movements such as yawning and chewing gum.
A key factor is also your food intake. A TMJ diet may be prescribed by your dentist to avoid hard, sticky, or chewy foods.
Avoid foods such as apples, carrots, or popcorn. Instead, choose a healthy diet that includes soft and mushy food like whole-wheat pasta, fish, mashed potatoes, scrambled egg, and others.
It can be beneficial to change small habits associated with your jaw.
- Avoid hard or chewy foods
- Reduce stress to avoid jaw clenching and other coping behaviors
- Avoid jaw movements that are accompanied by wide yawning and gum chewing.
TMJ pain can be managed with short-term nonsteroidal anti-inflammatory medications (NSAIDs). These medications are effective in reducing jaw pain and headaches. These include aspirin (Excedrin), naproxen (Aleve), and ibuprofen/Advil.
It can help with pain relief by icing your jaw. Jaw exercises can be used to relax your muscles and ease your symptoms.
Orthodontic Surgery
Orthodontic surgery is an option if lifestyle changes and medication don’t work. These procedures permanently change the shape of your teeth. Orthodontic surgery is not a permanent solution for TMJ headaches.
These surgeries can be performed by an experienced orthodontist. If you’re considering having surgery, it is important to be careful about who you choose as your orthodontist.
None of these treatments has been shown to be effective. TMJ headache pain is a serious condition that requires extreme caution. It is difficult to find a TMJ disorder specialist in medicine or dentistry.
Talking to a doctor at a university or hospital’s pain clinic might also be an option. This could be particularly helpful in diagnosing the source of TMJ pain.

