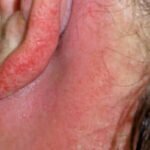
A rash behind ear can occur from a variety of causes and medical conditions. Certain viral infections and autoimmune diseases can cause a rash behind the ears in both children and adults. Some types of rash behind the ears caused by contact dermatitis are usually not concerning, but other causes, including rubella, ear eczema, and seborrheic dermatitis can be more serious. Here are all things you need to know about the causes, symptoms, and treatments for rashes behind the ears.
The delicate skin behind the ears is a common source of rashes. They can be hard to treat as you cannot see the affected area.
A rash behind your ears can be caused by many things, including skin irritation from haircare products and fungal infections.
Children and adults can get a rash behind their ears from viral infections or autoimmune diseases. Although some causes aren’t serious, like contact dermatitis or autoimmune diseases, there may be other more serious causes such as rubella.
We will be discussing the possible causes and treatment options for a rash behind your ear.
Table of Contents
What can cause a rash behind the ear?
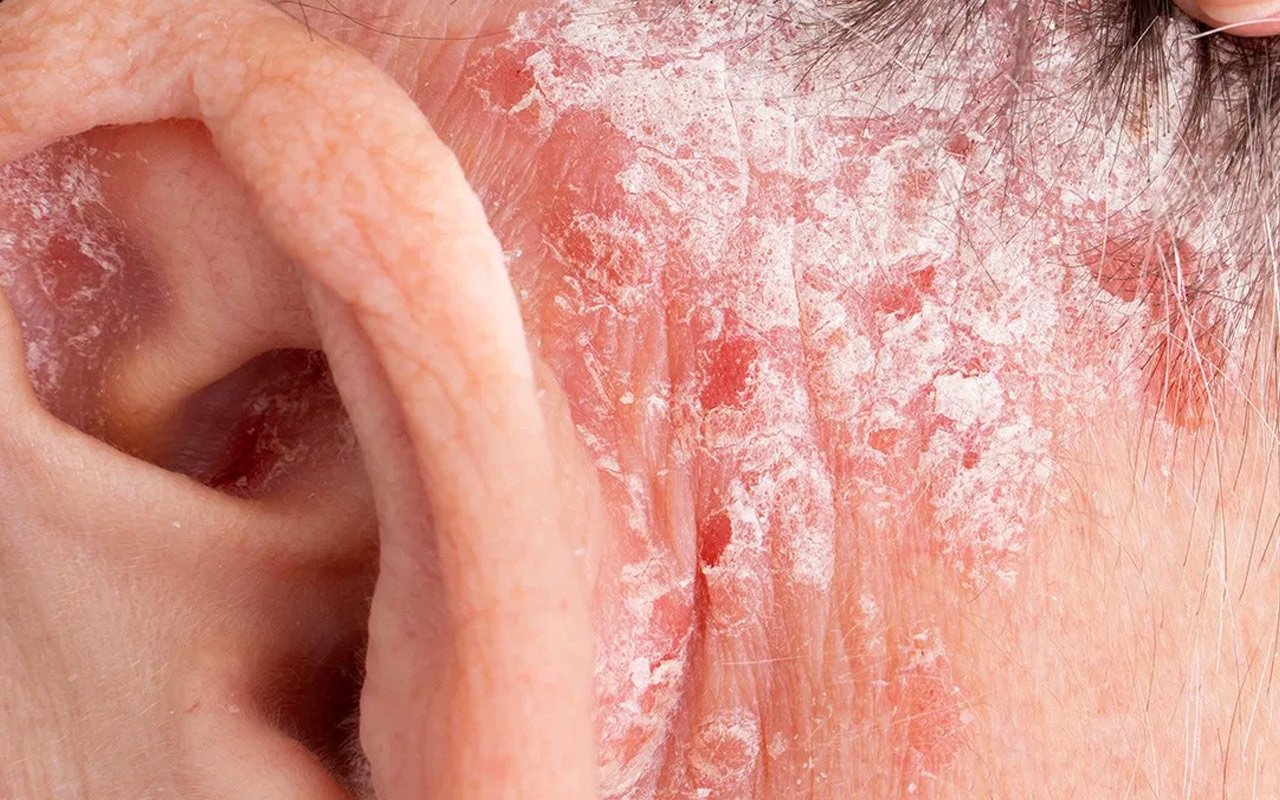
Itching behind the ears can cause redness, swelling, itching, and flaking of the skin. These symptoms can range from annoying to severe. These are the most common causes of a behind-the-ear rash.
Contact dermatitis
Contact dermatitis refers to an allergic reaction to a specific substance.
A rash may develop if an allergen-inducing substance is in contact with the skin behind the ears.
Contact dermatitis behind your ears can be caused by the following allergens:
- Shampoos
- Soaps
- Other hair care products
Paraphenylenediamine (PPD) is an example of a common contact allergen.
Symptoms
Contact dermatitis is a condition that causes itching, dryness, flaking, and irritation of the skin.
Diagnosis
A doctor will diagnose contact dermatitis by taking the patient’s medical history and performing a physical exam. The relevant medical history includes hobbies, medications, as well as the use of perfumes and fragrances.
The doctor will then assess the patient’s symptoms and perform a patch test.
Sometimes, they might need to do a biopsy in order to confirm their diagnosis.
Treatment
Avoiding the substance that causes the reaction or rash is the best treatment.
Sometimes, a doctor might recommend oral or topical corticosteroids to reduce itching and inflammation.
Itching may be relieved by prescription and over-the-counter oral antihistamines.
People may find that applying cold, or even wet soaks to their skin soothe them and reduces itching. You can also use moisturizers.
Rubella
Rubella, also known as German measles is a rare viral infection that can affect children and young adults.
A 2020 article states that rubella is usually self-limiting and benign. According to the Centers for Disease Control and Prevention, most rubella cases in children and adults are mild.
Rubella can be fatal in pregnant women if it develops within the first ten weeks. These complications include severe congenital abnormalities, pregnancy loss, and fetal death.
Symptoms
According to the CDC, 25-50% will have rubella symptoms.
If symptoms do occur, however, they will often differ between adults and children.
According to the CDC, children often get a rash on their faces that spreads to their bodies. It will last for about three days.
You may also experience other symptoms 1-5 days before you get a rash.
- A headache
- Low-grade fever
- It is uncomfortable
- A cough
- Swollen lymph nodes
- A mild case of pinkeye
- A runny nose
Rubella is a mild infection that affects adults. They have a sore neck and a low-grade fever. The rash first appears on the skin and then spreads to the entire body.
A person can be contagious starting 8 to 8 days before the rash occurs.
Diagnosis
Sometimes, the symptoms of rubella can be mild or nonspecific and doctors might find it difficult to diagnose based on a physical exam.
More accurate serology testing for rubella.
Doctors can test for antibodies to rubella-specific immunoglobulin M by using serology testing. These antibodies can be detected four days after the rash develops.
Treatment
Due to the 1969 introduction of a vaccine, rubella incidence has decreased in many countries.
Rubella is not curable. If you have symptoms, it is important to get prompt treatment.
Supportive treatments include fluids, antipyretics, and nonsteroidal anti-inflammatory drugs for fever and aches. These may be combined for some people.
Scalp psoriasis
People suffering from scalp psoriasis may have discolored patches of thickened skin behind their ears.
Plaques can get itchy and flake easily, giving rise to a dandruff appearance.
Symptoms
Other signs of scalp psoriasis are:
- Silvery-white Scales
- Dry scales
- Dry, cracked scalp
- Itching
- Pain
- Burning
- Hair loss
Diagnosis
Psoriasis can usually be diagnosed by doctors by looking at the lesions on your skin.
Treatment
Topical treatments are possible for people suffering from scalp psoriasis. They typically have minimal involvement of the rest.
If they have large lesions, people may need systemic medication.
Some people use topical agents to treat scalp psoriasis.
- Coal tar
- Vitamin D analogs
- Corticosteroids
- Other shampoos that contain oils or other ingredients to reduce symptoms
These treatments can be difficult to apply due to the hair on the heads. Some people might stop using these products as a result.
Although localized ultraviolet B therapy can be used in place of topical medication, it is more expensive and is not widely accessible.
Systemic drugs are not approved for the treatment of scalp psoriasis. These drugs include:
- Methotrexate
- Cyclosporin A
- Biotherapy
Measles
Measles is caused by the virus rubeola.
Measles can be contracted from others via airborne particles.
The measles skin rash is located behind the ears and along your hairline. It can affect the trunk, face, arms, legs, and trunk.
According to the CDC, measles can pose a danger.
Complications are more common in children under 5 years old and older adults. These complications can include diarrhea, pneumonia, or encephalitis. Encephalitis refers to inflammation of the brain.
Symptoms
Doctors outline the three stages of measles-infected persons: prodromal (eruptive), and convalescent.
People may experience the following symptoms during the prodromal stage:
- High fever
- Malaise
- Inflammation of the nasal passages
- Inflammation of the inner eyelids
- Dry cough
The eruptive stage is when the patient develops a rash around the ears and along the hairline. This can spread to the trunk, face, and extremities.
The rash will disappear in the exact same way it appeared in the final stage.
After the rash begins, fever and general malaise can be treated within 2 to 3 days.
Diagnosis
Doctors look at symptoms and how measles spreads in the community to diagnose measles. They also examine laboratory results.
A blood test can be used to check for certain immunoglobulins, and it can also be used to isolate the virus responsible.
Treatment
Getting vaccinated can help stop the spread of measles.
The CDC recommends that children get their vaccinations at 12-15 months old and a booster shot at 4-6 years.
Although there is no cure, doctors might prescribe medicine to treat measles.
Intertrigo
Intertrigo can happen at any age but is more common in older people. A person with a weak immune system is also at greater risk. Intertrigo behind the ears may occur in babies who drool while they sleep.
Intertrigo is when the skin rubs against another part of the skin that is moistened or frictional. The skin may become inflamed.
Intertrigo can also be caused by bodily secretions like saliva, sweat, and urine.
Symptoms
Intertrigo symptoms include:
- Flushed skin
- Itching
- Stinging
- A burning sensation
Diagnosis
To identify the type and severity of the rash, doctors need to inspect the skin.
A careful examination could reveal secondary fungal or bacterial infections that will require additional treatment.
Treatment
There are several first-line options for treatment:
- Zinc oxide ointments
- Petrolatum
- Talcum powder
- Aluminum sulfate
- Calcium acetate solution
- Low potency corticosteroids
If the doctor diagnoses secondary fungal or bacterial infections, the patient may need antibacterial or antifungal treatment.
- Topical erythromycin
- Topical clindamycin
- Chlorhexidine
- Whitfield’s ointment
- Topical mupirocin
There are some infections that may require oral antibiotics such as penicillin or clindamycin. Oral antifungal agents such as fluconazole might also be required.
COVID-19
COVID-19 can also be the cause of a rash behind the ears. Dermatologists have seen measles-like bumps on the chest, back, ears, and other areas of COVID-19 patients.
Although unproven because large enough research data are not available, some recent studies suggest the possibility of skin rash as a clinical manifestation of coronavirus disease 2019 (COVID-19).
The rash can last for weeks while you are recovering from COVID. A large and itchy rash with small lumps and blisters may appear during COVID or several weeks later.
Some people may develop a widespread maculopapular rash (a flat or raised skin discoloration), while others may develop hives. This type of COVID-19 rash can appear with blisters that look like chickenpox.
Currently, reports show that a covid rash usually lasts 2 to 12 days, with most people having a rash for 8 days.
You can take care of your COVID-19 rash at home by applying cool compresses and using over-the-counter topical products. To relieve pain or itching, apply hydrocortisone cream to the affected area.
Rash behind the ear in a baby and toddler
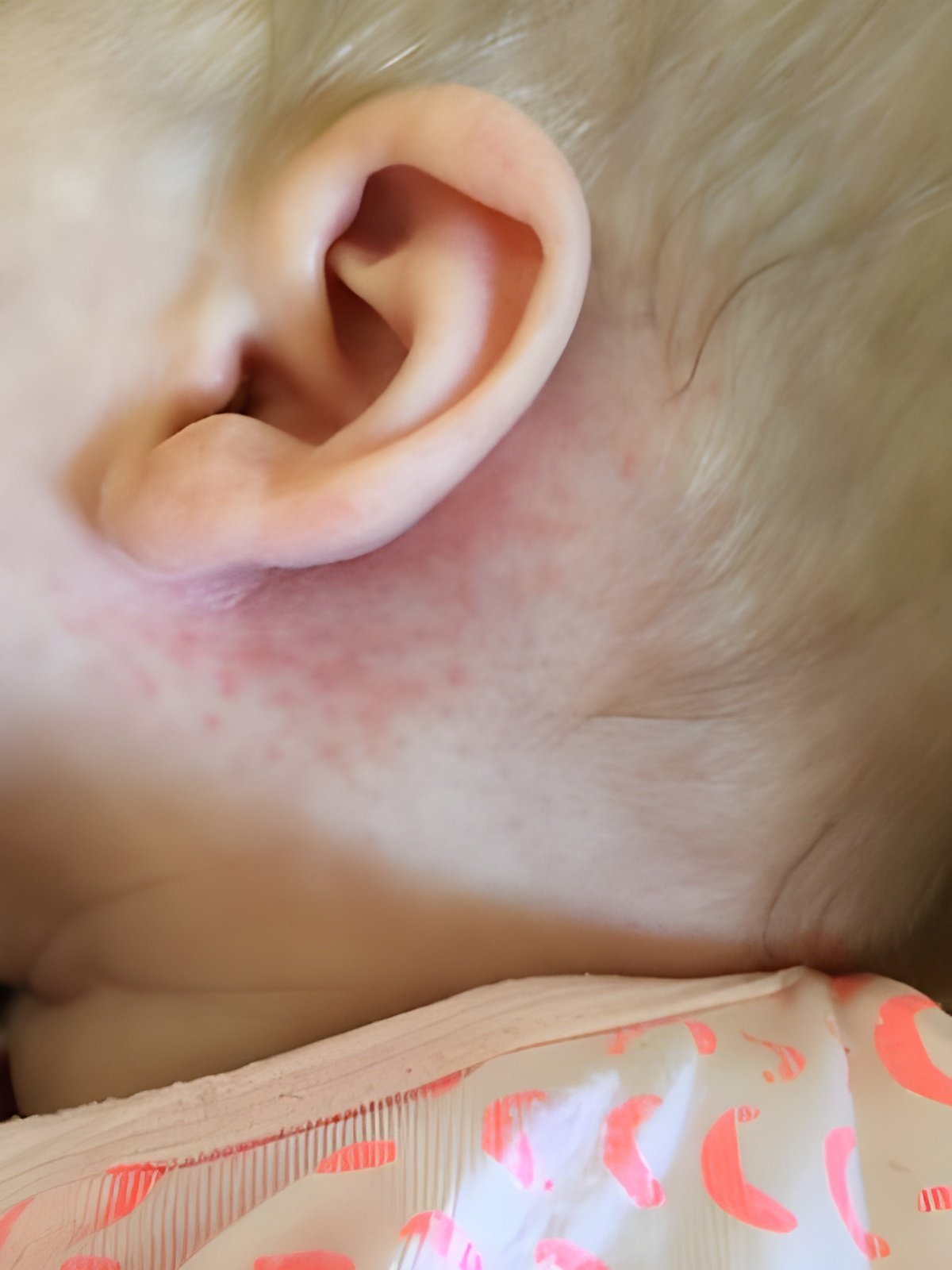
Rashes behind the ears in babies or toddlers are also common, and treatment is fairly straightforward. Children as young as two years old can get rashes behind their ears from conditions that adults do not normally experience.
Intertrigo behind the ears is one example. This skin condition can occur in the skin folds. Sometimes, a baby’s drool goes behind its ears. It can cause the skin to become hot, red, and painful.
Intertrigo can be treated by parents using zinc creams and other moisture barriers to prevent skin from becoming damaged.
Foot, hand, and mouth disease is another condition that can lead to a rash behind your ears. This is a common condition in preschools and childcare centers.
Heat rashes are caused by blockage and inflammation of the sweat ducts when heat and humidity are high, causing: tiny red bumps. Itching and tingling sensations. redness and slight swelling of the affected area.
Heat rash behind the ear is an itchy skin condition that affects the skin behind the ear, as well as most areas of the ear. This is a common disease in children.
The causes of heat rash behind the ears are many, but the main cause is a blockage and inflammation of sweat ducts in heat and high humidity, which causes: tiny red spots. an irritating itch and prickling sensation, redness, and mild swelling of the affected area.
Extremely hot weather or allergies to shampoos or skin care products can also cause heat rash behind the ears. Most cases of heat rash will clear up on their own within a few days with appropriate home care.
A child might also have a red, blistering skin condition, as well as a fever and a runny nose.
Seborrheic Dermatitis ( cradle cap), another condition that can affect babies, is also possible.
Cradle cap
Seborrheic dermatitis is another name for cradle cap. Cradle cap is a skin condition that usually appears in infants, usually between 1-2 months of age. The scalp appears oily, and yellow and may be accompanied by an irritating red rash on the face, behind the ears, on the neck, and even under the armpits.
Symptoms
The following symptoms may be experienced in infants with cradle caps:
- The yellow crust on the skin
- Flushed skin with yellow or white flakes
- Inflammation
Although the cradle cap is not likely to cause agitation in babies, parents and caregivers should inspect the scalp for signs of infections.
Diagnosis
Because cradle caps can be caused by other skin conditions, doctors will examine infants with cradle caps.
Babies with cradle caps will have thick, greasy skin that does not cause itching.
Other conditions that could resemble cradle caps are:
- Eczema
- Fungal infections
- Psoriasis
- Rosacea
Treatment
The United Kingdom’s National Health Service states that a caregiver or parent can:
- Regularly wash your infant’s hair with baby shampoo
- Use a soft brush to gently brush your scalp
- Apply baby oil, vegetable oil, or petroleum jelly to the affected areas at the night. Wash them the next morning with baby shampoo
Avoid using soap, peanut oil, or adult shampoos. As this could lead to infection, they should avoid picking at the crusts.
Rash behind the ears: Treatment
The underlying cause of rashes behind the ears will determine the treatment. The best way to cure a rash behind the ears is to keep your skin dry, clean, and moisturized.
Medical treatment
If the rash behind your ears is caused by a fungal infection or bacterial disease, a doctor might prescribe treatment. A fungal rash is often red and itches or burns. This fungus infection causes pain and itching. The infection can also cause a feeling of fullness in the ear and sometimes hearing loss.
It’s important to remember, otomycosis is a fungal infection that affects one or sometimes both ears. It mainly affects people living in warm or tropical areas. It also can affect people who regularly swim, have diabetes, or have other chronic skin conditions.
These treatments include topical antifungal medications or oral antibiotics. This is especially true when the skin is infected, bleeding, cracked, or damaged.
Your doctor will likely prescribe antifungal ear drops. They may contain clotrimazole, fluconazole, or miconazole. Scientific research proves that clotrimazole drops, miconazole cream, and fluconazole drops have the same effect.
You can also use apple cider vinegar to treat fungal infections behind the ears. Known for its ability to fight chronic yeast infections, apple cider vinegar can also kill the fungi that cause ear infections.
To use apple cider vinegar for ear infections, mix one part apple cider vinegar with one part water. Dip a cotton ball in the solution, then use a cotton pad soaked in the apple cider vinegar solution to clear the rash. This is the best home treatment for rash behind the ears caused by a fungal infection
Home remedies
Avoiding the allergen that causes the rash may help reduce its appearance. These are some home remedies that might help.
- Use warm water and soap to clean the area. Always wash your hands after touching the rash.
- Use a non-fragranced anti-itch cream or a fragrance-free skin lotion depending on your symptoms. Cover the area lightly with a bandage and allow the skin to breathe.
- Avoid scratching the affected areas.
- For swelling behind the ears, apply cloth-covered compressions.
How to diagnose a rash behind the ear?
Sometimes, a doctor can diagnose skin rash by looking at the affected area and taking a history.
A doctor may send a sample of the skin to a laboratory if they are unsure what is causing it. The rash can be identified by a laboratory technician.
When to see a doctor?
The rash can be caused by many medical conditions. Undiagnosed rashes are best treated by a physician or another healthcare provider.
Additional symptoms such as fever, malaise, or nausea may indicate an infection. You should seek immediate medical attention.
A rash can become infected if it is scratched repeatedly. A doctor should be consulted if you have a rash or develop an infection.
Rashes can appear behind the ears due to different skin conditions like contact dermatitis or psoriasis.
A rash may occur in people who have measles or rubella infections. Infants with rash behind the ears are more likely to have intertrigo or cradle caps.
If a rash develops along with other symptoms such as fever or severe discomfort, it should be treated immediately.
Rash behind the ears: Pictures
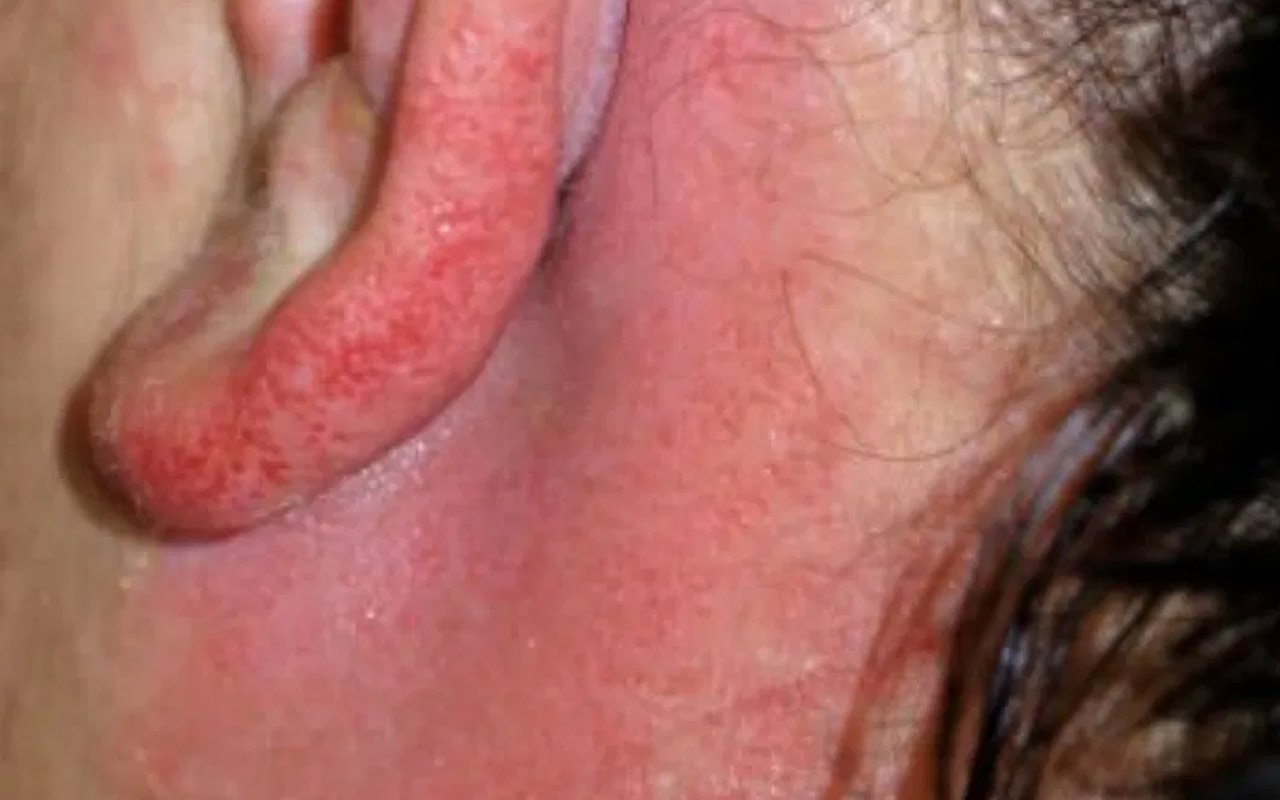
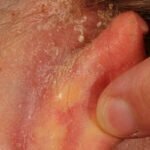
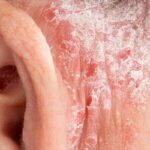
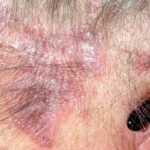
Here are some pictures of the rash behind the ear.
- What can cause a rash behind the ear?
- rash behind the ears
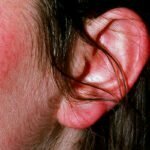
- red rash of measles
- Lichen planus lesions are known to be purplish.
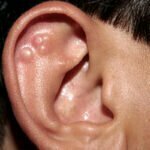
- Granuloma annulare is very common. It presents as skin-colored, round lesions and is noncancerous.
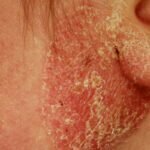
- Fungal infections can be transmitted from an animal to humans.
- A lupus rash isn’t itchy and appears as red bumps on sun-exposed areas of skin.
- Rash Behind Ear